Mastering Fundus Examination: A Comprehensive Guide to Key Retinal Findings

A meticulous fundus examination serves as a window into both ocular health and systemic well-being. By evaluating the posterior pole and mid-periphery, clinicians can detect early markers of hypertension, carotid artery disease, and even neurological emergencies.
This guide breaks down the most significant clinical findings seen during ophthalmoscopy, providing a high-yield review for students and practitioners alike.
Common Vascular Manifestations
Retinal vasculature is often the first place where systemic vascular disease becomes visible.
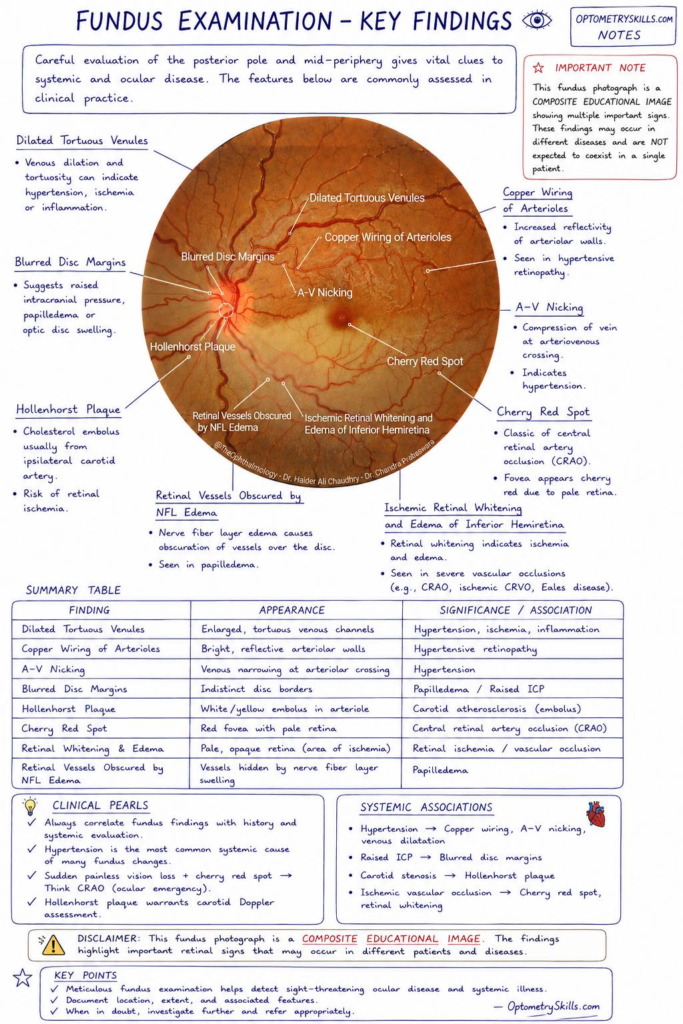
- Copper Wiring of Arterioles: As arteriolar walls thicken due to chronic hypertension, their light reflex increases, taking on a metallic, “copper” appearance.
- A-V Nicking: This occurs when a thickened arteriole compresses a vein at a common adventitial crossing, a hallmark of hypertensive retinopathy.
- Dilated Tortuous Venules: Often a sign of venous stasis, these can indicate impending vascular occlusion, ischemia, or underlying inflammatory conditions.
Identifying Critical Retinal Lesions
Certain findings act as “red flags” that require immediate systemic investigation or emergency referral.
Hollenhorst Plaque
A Hollenhorst plaque is a refractile, orange-yellow cholesterol embolus typically originating from the ipsilateral carotid artery. Finding one warrants an urgent carotid Doppler to assess the risk of a future stroke or retinal branch artery occlusion.
Cherry Red Spot
The classic cherry red spot is the clinical signature of a Central Retinal Artery Occlusion (CRAO). The fovea appears bright red in contrast to the surrounding pale, edematous retina, which has lost its blood supply. This is an ocular emergency.
Disc Margins and Nerve Fiber Layer (NFL) Edema
Evaluating the optic disc is essential for ruling out raised intracranial pressure (ICP).
- Blurred Disc Margins: Indistinct borders of the optic nerve head can suggest papilledema or optic disc swelling.
- NFL Edema: Nerve fiber layer edema can obscure the retinal vessels as they cross the disc margin, a key sign in progressing papilledema.
Clinical Pearls for the Exam Room
- Correlate with History: Always match fundus findings with the patient’s systemic history (e.g., blood pressure, carotid health).
- Sudden Vision Loss: Any sudden, painless loss of vision coupled with a cherry red spot must be treated as a CRAO until proven otherwise.
- Documentation: Always document the location, extent, and associated features of any lesion for longitudinal monitoring.
Summary Table: Retinal Findings at a Glance
Finding Appearance Primary Association Copper Wiring Bright, reflective arteriolar walls Hypertensive Retinopathy A-V Nicking Venous narrowing at crossing Chronic Hypertension Hollenhorst Plaque Yellow/refractile embolus Carotid Atherosclerosis Cherry Red Spot Red fovea with pale retina CRAO (Emergency) Blurred Margins Indistinct disc borders Raised ICP / Papilledema References & Credits
This article is based on clinical standards outlined in Vaughan & Asbury’s General Ophthalmology. Image
notes is made by OptometrySkills.com.
Fahmina is a qualified optometrist. She founded OptometrySkills.com to make professional-grade eye care knowledge accessible to practitioners and patients alike.
