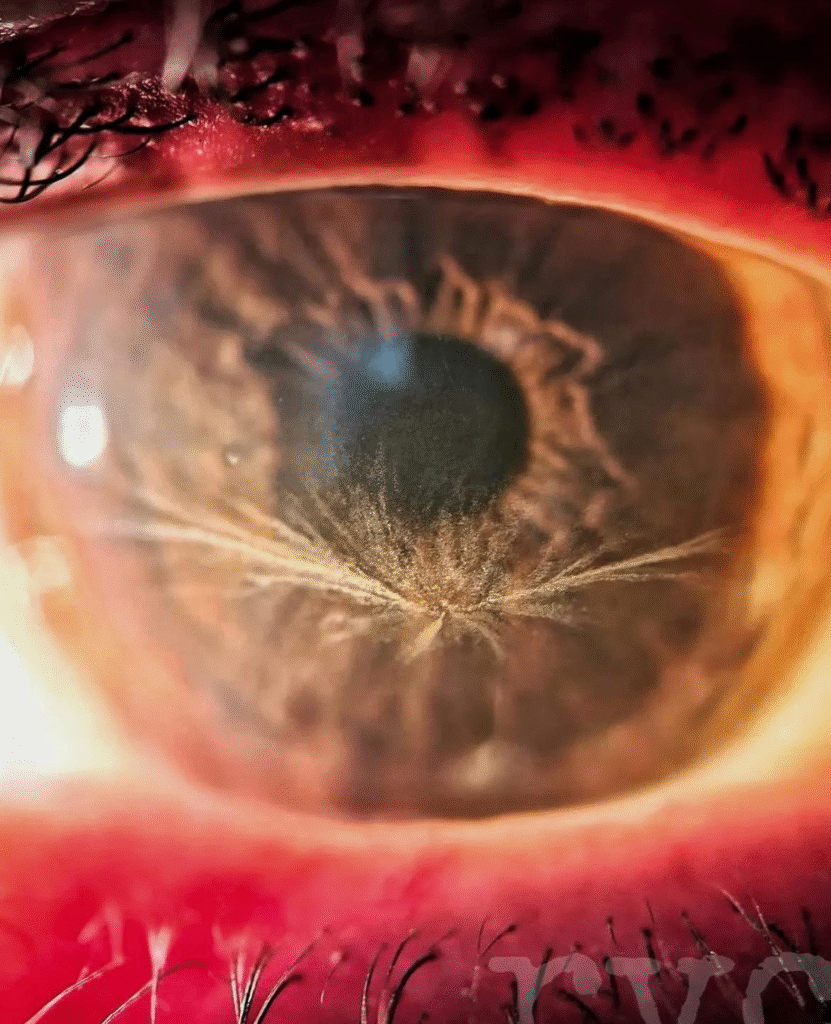
Vortex keratopathy, also known as corneal verticillata, is a distinctive corneal finding characterized by fine, golden-brown or gray, whorl-like epithelial opacities radiating in a spiral pattern from a central point, typically inferior to the visual axis. The term “verticillata” derives from the Latin word verticillus meaning “whorl.” Although the condition is often benign and asymptomatic, its presence is clinically significant because it can serve as a marker for systemic drug exposure or metabolic storage diseases.

Pathogenesis
The characteristic whorl pattern arises due to the centripetal migration of corneal epithelial cells from the limbus toward the center of the cornea. Lipid-soluble medications or metabolic substrates accumulate within lysosomes of basal epithelial cells as lamellar inclusion bodies. The corneal epithelial turnover and limbal stem cell migration cause these deposits to align along vortex-like lines.
These deposits do not typically affect the stromal or endothelial layers, and corneal transparency is generally preserved. The severity of the deposits correlates with drug dose, treatment duration, and individual metabolic clearance.
Etiology
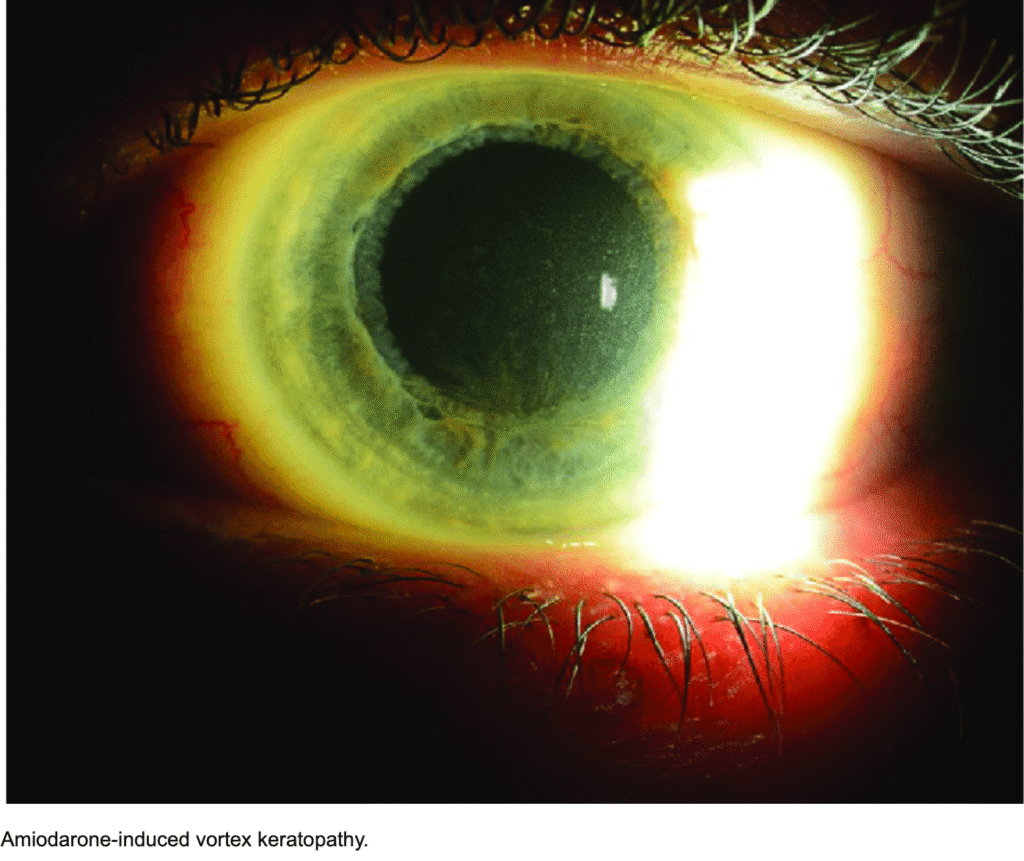
Image source
1. Drug-Induced Vortex Keratopathy
This is the most frequent cause. Several medications have been implicated:
- Amiodarone: The most classic and well-documented cause. Up to 90% of patients on long-term therapy (typically >200 mg/day for several months) develop corneal verticillata. Deposits appear after 3–6 months of therapy and may persist for months after discontinuation.
- Chloroquine and Hydroxychloroquine: Used in malaria prophylaxis and autoimmune disorders such as systemic lupus erythematosus and rheumatoid arthritis. Deposits arise due to drug-lipid complex formation within corneal epithelial lysosomes.
- Tamoxifen: Used in breast carcinoma; associated with vortex keratopathy and crystalline retinopathy.
- Indomethacin, Chlorpromazine, Phenothiazines, Suramin, and Fabrazyme have also been occasionally reported.
2. Metabolic and Inherited Disorders
- Fabry Disease (Anderson–Fabry Disease): An X-linked lysosomal storage disorder caused by deficiency of α-galactosidase A enzyme, leading to sphingolipid accumulation in multiple organs. Corneal verticillata is one of its earliest ocular manifestations, seen in up to 90% of male patients and many female carriers.
Clinical Features
- Appearance: Whorl-shaped, gray-brown or golden epithelial deposits radiating from the center, usually sparing the limbus.
- Laterality: Typically bilateral and symmetrical.
- Symptoms: Most patients are asymptomatic. Rarely, mild halos, glare, or blurred vision may occur in severe cases.
- Course: Lesions appear gradually and are non-inflammatory; the corneal surface remains smooth with no epithelial defect.
Diagnostic Evaluation
1. Slit-Lamp Biomicroscopy:
The main diagnostic tool. Deposits are best visualized with oblique illumination and high magnification.
2. Fluorescein Staining:
Negative; there is no epithelial loss.
3. In Vivo Confocal Microscopy (IVCM):
Reveals highly reflective, intracellular inclusions within basal epithelial cells, confirming intra-epithelial deposition.
4. Differential Diagnosis:
- Hudson-Stähli line
- Fleischer ring (in keratoconus)
- Epithelial basement membrane dystrophy
- Iron deposition lines from chronic exposure or trauma
Management and Prognosis
- Drug-induced cases:
- No treatment is required in most cases as vision is rarely affected.
- If visual symptoms develop or if systemic toxicity is suspected, the prescribing physician may reduce dosage or discontinue the drug.
- Deposits typically fade over several months after drug cessation.
- Fabry disease:
- Corneal verticillata is a diagnostic clue prompting systemic evaluation.
- Enzyme replacement therapy (ERT) may slow systemic progression, though corneal findings often persist.
- Refractive surgery:
- Presence of vortex keratopathy should be noted but does not usually contraindicate procedures such as LASIK unless significant visual disturbance exists.
Prognosis and Clinical Relevance
Vortex keratopathy is a benign, non-inflammatory condition with minimal impact on visual acuity. Its primary importance lies in its diagnostic and pharmacovigilant value. Recognition of this pattern during routine slit-lamp examination should prompt a detailed drug history and, in relevant cases, systemic evaluation for Fabry disease.
Key Clinical Pearls
- Whorl pattern = epithelial migration direction.
- Common with amiodarone, chloroquine, hydroxychloroquine.
- Deposits are reversible with drug cessation in acquired forms.
- Acts as an ocular biomarker for systemic disorders like Fabry’s disease.
References
- Sahyoun M, et al. Drug-induced corneal deposits: An up-to-date review. Clin Ophthalmol. 2022;16:1001–1016. PMC8961126
- American Academy of Ophthalmology. EyeWiki: Cornea Verticillata. https://eyewiki.org/Cornea_Verticillata
- Fraunfelder FT, et al. Corneal Verticillata: Drug and Metabolic Associations. Surv Ophthalmol. 1982;26(1):1–15.
