Index
Notes on Vernal Keratoconjunctivitis (VKC) or Spring Catarrh

Vernal Keratoconjunctivitis (VKC) is a chronic, recurrent, bilateral, interstitial, allergic inflammation of the conjunctiva that shows seasonal recurrence—most often during warm months.
It is self-limiting, but can lead to corneal complications that may threaten vision if untreated.
Synonyms
- Spring Catarrh
- Warm-Weather Conjunctivitis
- Vernal Conjunctivitis
Nature of the Disease
- Recurrent and bilateral.
- Non-infectious (allergic in origin).
- Has a distinct seasonal pattern, particularly in spring and summer.
- Involves both conjunctiva and cornea in varying degrees.
- Self-limiting, generally subsides after puberty.
Etiopathogenesis
1. Immunological Mechanism
VKC represents a complex allergic disorder involving both:
- Type I Hypersensitivity (IgE-mediated): Immediate hypersensitivity to airborne allergens such as pollen, dust, and animal dander.
- Type IV Delayed Hypersensitivity: Chronic cellular infiltration and tissue remodeling mediated by Th2 lymphocytes and cytokines (IL-4, IL-5, IL-13).
2. Cellular Pathways
- Mast Cells → Degranulate to release histamine, leukotrienes, prostaglandins → acute itching, redness, chemosis.
- Eosinophils and Basophils → Release toxic proteins (e.g., major basic protein) → epithelial damage → shield ulcer.
- Th2 Lymphocytes → Produce IL-4 and IL-13 promoting IgE synthesis; IL-5 stimulates eosinophil activation.
- Fibroblasts and vascular changes → papillary hypertrophy and scarring.
3. Immunoglobulin E (IgE) and Histamine Role
- Elevated tear IgE levels in active VKC.
- Histamine causes itching, hyperemia, and vascular permeability.
Predisposing Factors
- Age: Commonly between 4 – 20 years.
- Sex: Markedly more common in boys (ratio ≈ 3 – 4 : 1).
- Season: Peaks in spring and summer; rare in winter.
- Climate: More prevalent in tropical and subtropical areas; rare in cold climates.
- Atopy: Often associated with eczema, asthma, allergic rhinitis or family history of atopy.
- Socio-environmental: Dusty, windy, sun-exposed environments increase recurrence.
Pathology
Conjunctival Changes
- Epithelial hyperplasia with downward projections into the subepithelial tissue.
- Adenoid layer infiltration with eosinophils, plasma cells, lymphocytes, and histiocytes.
- Fibrous layer proliferation → hyaline degeneration → papilla formation.
- Blood vessels: Dilated, permeable, and proliferated → chemosis and congestion.
Corneal Changes
- Punctate epithelial erosions.
- Shield ulcer formation.
- Plaque formation.
- Limbal infiltration and pseudogerontoxon.
Clinical Features
Symptoms
- Intense itching: hallmark symptom, aggravated by heat and wind.
- Burning and foreign-body sensation.
- Photophobia and lacrimation.
- Thick ropy (mucoid) discharge.
- Heaviness of eyelids and drooping appearance.
Signs
VKC manifests in three main clinical forms:
1. Palpebral (Form)
- Involves upper tarsal conjunctiva bilaterally.
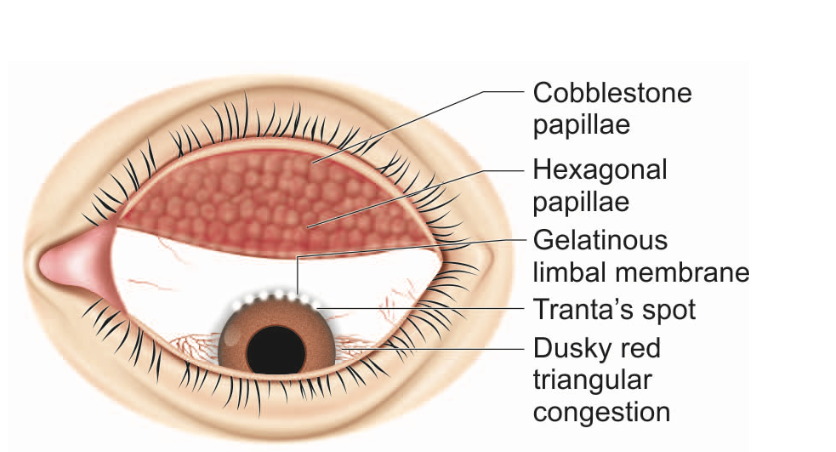
- Typical lesion: Large, flat-topped papillae arranged in a cobblestone or pavement-stone pattern.
- Color: Grayish-pink elevations.
- Severe cases: Papillae may become hypertrophic → “Giant Papillae”.
- Discharge: Thick, ropy, whitish mucus.
- Associated: Hyperemia, lid oedema, ptosis.
2. Bulbar (Limbal) Form
- Dusky-red triangular injection near the limbus.
- Gelatinous thickened mass around the limbus.
- Tranta’s spots: Small white raised dots — accumulations of eosinophils and epithelial debris at limbus.
- More common in dark-skinned individuals (e.g., African, Indian populations).
3. Mixed Form
- Features of both palpebral and bulbar types.
- Common in moderate to severe VKC.
Corneal Involvement (Vernal Keratopathy)
Corneal changes occur in ~6–30 % of patients.
| Type | Description / Features |
|---|---|
| 1. Punctate Epithelial Keratitis | Fine superficial epithelial erosions in upper cornea that stain with fluorescein and rose bengal. Results from mechanical friction of papillae. |
| 2. Shield Ulcer | Shallow transverse ulcer in upper cornea due to macro-erosions and eosinophil toxicity. Serious complication; predisposes to secondary bacterial infection. |
| 3. Vernal Corneal Plaque | White coating of fibrin and degenerating epithelium over healing ulcer — seen as an opaque plaque. |
| 4. Subepithelial Scarring | Ring-shaped opacity after repeated inflammation. |
| 5. Pseudogerontoxon | Peripheral lipid deposition near limbus forming a “cupid’s bow” appearance. |
Course and Prognosis
- Chronic and recurrent, lasting 5–10 years.
- Peaks in late childhood and early teens.
- Spontaneous resolution after puberty in most cases.
- Vision-threatening complications possible if corneal ulcer occurs.
- Not contagious.
Differential Diagnosis
| Condition | Differentiating Features |
|---|---|
| Trachoma | Follicles present on upper tarsal conjunctiva; scarring and Herbert’s pits common. |
| Atopic Keratoconjunctivitis | Occurs in older patients (> 20 yrs); associated with eczema of eyelids. |
| Giant Papillary Conjunctivitis | Related to contact lens use or foreign body; no seasonal pattern. |
| Phlyctenular Keratoconjunctivitis | Localized phlycten lesions with ulceration and photophobia; delayed hypersensitivity to tubercular protein. |
Investigations
- Eosinophilia in tears or conjunctival scrape.
- Elevated serum IgE levels.
- Conjunctival smear: Eosinophils and mast cells.
- Tear film tests: Often show reduced stability.
- In vivo confocal microscopy: Demonstrates inflammatory cell infiltrate.
Complications
- Corneal shield ulcer → scarring → vision loss.
- Steroid-induced glaucoma or cataract if steroids misused.
- Keratoconus association (chronic eye rubbing).
- Secondary bacterial keratitis.
Treatment
A. Topical Anti-inflammatory Therapy
- Corticosteroids: (Fluorometholone, Medrysone, Dexamethasone)
- Rapid control of inflammation.
- Short course under IOP monitoring.
- Mast Cell Stabilizers: (Sodium Cromoglycate 2%, Lodoxamide 0.1%)
- Prevent mast cell degranulation; use prophylactically.
- Dual-Action Agents: (Azelastine, Olopatadine, Ketotifen)
- Antihistaminic + mast cell stabilizing effect; excellent for long-term control.
- NSAID Drops: (Ketorolac, Diclofenac)
- Symptomatic relief of pain and inflammation.
- Immunomodulators: (Cyclosporine 0.5–1%, Tacrolimus 0.03%)
- Used in severe or steroid-resistant cases as steroid-sparing agents.
B. Lubricating and Mucolytic Therapy
- Artificial tears (carboxymethyl cellulose or hydroxypropyl methylcellulose) → comfort and tear film stability.
- Acetyl Cysteine 0.5 % → breaks down mucoid plaque and ropy discharge.
C. Systemic Therapy
- Oral Antihistamines: (Cetirizine, Loratadine) for itching relief.
- Short course of oral steroids: only for very severe unresponsive cases.
D. Management of Giant Papillae
- Supratarsal injection of long-acting steroid (e.g., triamcinolone).
- Cryotherapy or Surgical excision if mechanically irritating cornea.
E. General Measures
- Avoid rubbing eyes.
- Use cold compresses and dark goggles for symptom relief.
- Maintain clean, dust-free environment.
- Relocation to cooler climate in severe chronic cases can help.
F. Treatment of Vernal Keratopathy
| Lesion | Management |
|---|---|
| Punctate Keratitis | Increase frequency of topical steroids and lubricants. |
| Shield Ulcer | Debridement of necrotic epithelium ± bandage contact lens or amniotic membrane transplant. |
| Corneal Plaque | Superficial keratectomy to remove plaque. |
| Non-healing ulcer | Excimer laser therapeutic keratectomy (PTK) may be needed. |
G. Desensitization and Allergen Control
- Allergen avoidance is key.
- Immunotherapy has shown limited benefit but may be tried in refractory atopic patients.
Follow-Up and Optometrist’s Role
- Monitor IOP during steroid therapy.
- Educate patients about avoiding eye rubbing.
- Recommend UV-protective sunglasses.
- Identify early signs of keratoconus and refer promptly.
- Reinforce compliance with maintenance therapy to prevent exacerbations.
Prognosis
- Usually self-limiting; resolves after puberty.
- Chronic cases require long-term maintenance therapy.
- With proper management, visual prognosis is good; however, untreated shield ulcers can lead to permanent corneal scarring.
Summary Table
| Aspect | Key Points |
|---|---|
| Type | Allergic (Keratoconjunctivitis) |
| Onset | Childhood (4–20 yrs) |
| Laterality | Bilateral |
| Season | Warm months / spring |
| Symptoms | Itching, burning, ropy discharge, photophobia |
| Signs | Cobblestone papillae, Tranta’s spots, shield ulcer |
| Treatment | Steroids, mast cell stabilizers, antihistamines, immunomodulators |
| Complications | Corneal ulcer, scarring, secondary infection, glaucoma (due to steroids) |
