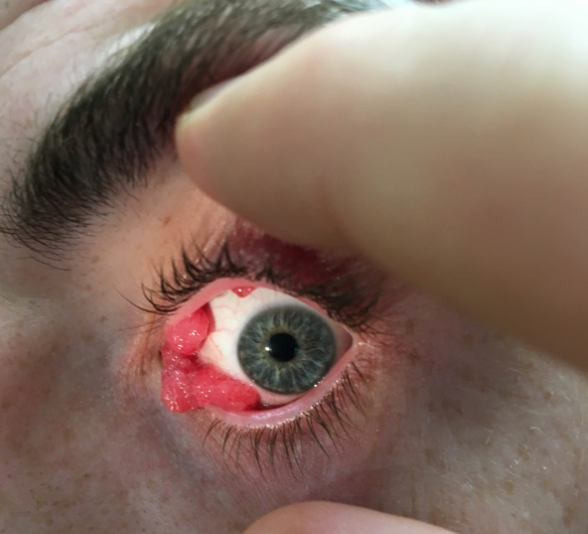
Types of Conjunctival papilloma
Conjunctival papilloma is a benign, epithelial tumor of the conjunctiva commonly encountered in clinical practice. Although non-malignant, its association with human papillomavirus (HPV), potential for recurrence, and occasional transformation into dysplastic lesions make accurate diagnosis and management essential for optometrists and ophthalmic professionals.
Understanding the lesion’s characteristic appearance, risk factors, and treatment options ensures timely referral and optimal patient outcomes.
What Is Conjunctival Papilloma?
A conjunctival papilloma is a benign epithelial neoplasm arising from the conjunctival mucosa.
It is characterized by papillary or lobulated epithelial projections supported by fibrovascular cores.
Histologically, it represents:
- Squamous epithelial hyperplasia
- Fibrovascular stromal core
- Often HPV-related koilocytotic changes
Although benign, it may grow, recur, or cause cosmetic concerns.
Etiology and Risk Factors of Conjunctival papilloma
1. HPV Infection
The most common cause.
- HPV types 6 and 11 → associated with benign papillomas
- HPV types 16 and 18 → rarely associated with dysplastic or pre-malignant changes
Transmission routes may include:
- Hand-to-eye contact
- Auto-inoculation
- Perinatal transmission in children
2. Chronic Irritation
Such as:
- UV exposure
- Smoking
- Ocular surface inflammation
3. Immunosuppression
May increase recurrence risk.

Types of Conjunctival Papilloma
1. Pedunculated Papilloma
- Most common form
- Pink, fleshy, vascular
- Finger-like projections
- Highly mobile
- Often located on inferior palpebral conjunctiva or caruncle
2. Sessile Papilloma
- Broad base
- Flatter, less mobile
- May have keratinized surface
- Slightly higher concern for dysplasia
3. Inverted Papilloma (rare)
- Grows inward into the substantia propria
- Higher risk of recurrence
- Considered pre-malignant in some cases
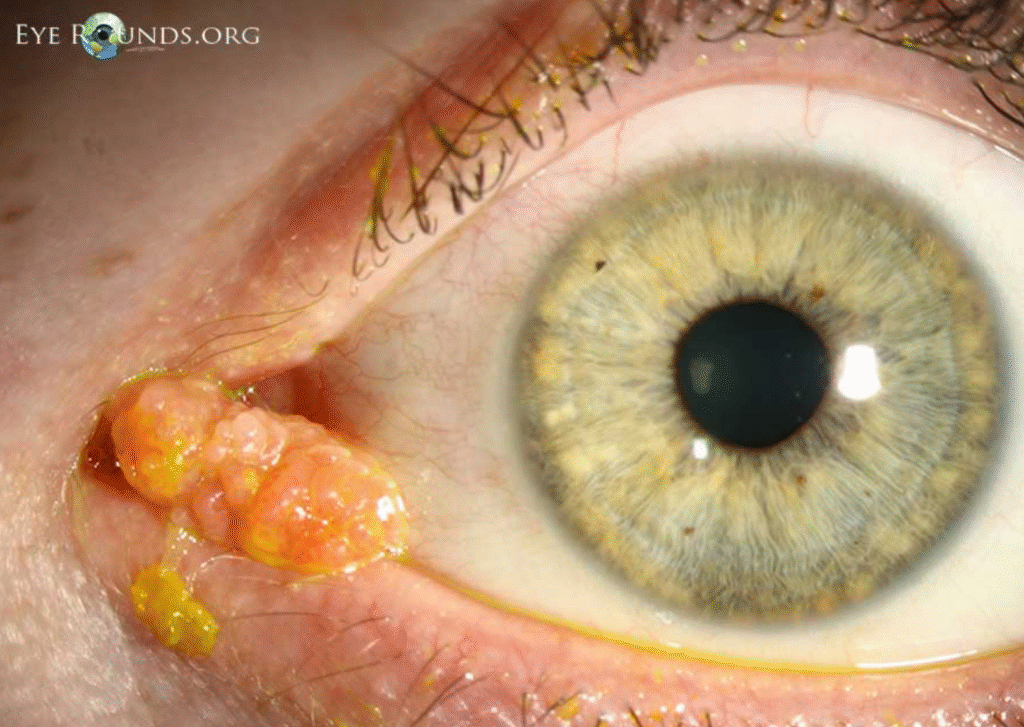
Clinical Presentation
Patient may report:
- A painless, growing mass
- Foreign body sensation
- Cosmetic concern
- Intermittent irritation
- History of viral warts elsewhere
On slit-lamp, the lesion appears:
- Pink, vascular, lobulated mass
- Surface may show papillary fronds
- Prominent feeder vessels
- May move with gentle pressure (pedunculated)
- Often located at:
- Caruncle
- Palpebral conjunctiva
- Bulbar conjunctiva near limbus
Differential Diagnosis
| Condition | Key Differentiating Features |
|---|---|
| Conjunctival Papilloma | Papillary mass, vascular core, often pedunculated |
| Conjunctival Intraepithelial Neoplasia (CIN) | Leukoplakia, gelatinous mass, feeder vessels, sessile |
| Pyogenic Granuloma | Smooth, red, highly vascular, rapid growth |
| Dermoid / Lipodermoid | Congenital, yellowish, at limbus or fornix |
| Papillomatous Conjunctivitis | Bilateral, associated with allergies |
Diagnosis
Diagnosis is primarily clinical, supported by:
1. Slit-lamp Biomicroscopy
Key to ruling out CIN or malignant transformation.
2. HPV Testing (optional)
Used in atypical, recurrent, or suspicious lesions.
3. Histopathology
Required when:
- The lesion is sessile
- Atypical appearance
- Rapid growth
- Concern for dysplasia
Management and Treatment Options
1. Observation
Appropriate if:
- Small, asymptomatic lesion
- Typical appearance
- No rapid growth
Children often show spontaneous regression.
2. Surgical Excision
The preferred treatment for:
- Cosmetic reasons
- Large lesions
- Recurrent lesions
- Suspicion of dysplasia
- Surface keratinization
No-touch technique is recommended to reduce recurrence.
3. Adjunctive Therapies (to prevent recurrence)
Cryotherapy
Applied to the base after excision.
Mitomycin-C (MMC)
Used in cases with dysplasia or recurrent lesions.
Interferon α-2b
- Topical or injected
- Very effective for diffuse or recurrent papillomas
- Especially useful in children to avoid surgery
CO₂ Laser / Radiofrequency Ablation
Used selectively.
4. Management of HPV
Advise patients on:
- Avoiding ocular rubbing
- Hand hygiene
- Treatment of periocular warts
Complications
- Recurrence (most common)
- Scarring after aggressive excision
- Malignant transformation (rare, usually associated with HPV 16/18)
- Cosmetic concerns
- Conjunctival irritation
Follow-Up
Recommend:
- 6–12 month follow-up for typical benign lesions
- 3–6 month follow-up for recurrent or atypical cases
- Immediate review if:
- Rapid enlargement
- Keratinization
- New pain, bleeding, or surface changes
Key Points for Optometrists
- Most conjunctival papillomas are benign and HPV-related.
- Pedunculated lesions are typical and usually harmless.
- Sessile or keratinized lesions require careful evaluation.
- Excision combined with cryotherapy or interferon significantly reduces recurrence.
- Always consider CIN in atypical or suspicious lesions.
Frequently asked questions
1. Is conjunctival papilloma caused by HPV?
Yes. Most conjunctival papillomas are associated with HPV types 6 and 11, which are considered low-risk strains.
2. Can conjunctival papilloma turn cancerous?
Malignant transformation is rare, but sessile or atypical lesions can show dysplasia. Suspicious lesions should always be biopsied.
3. How is conjunctival papilloma treated?
Treatment options include:
- Observation
- Interferon α-2b drops
- Surgical excision
- Cryotherapy
- Mitomycin-C in selected cases
4. Does conjunctival papilloma come back after removal?
Yes. Recurrence occurs in 10–30% of cases, especially when the base is not treated or when the lesion is HPV-positive.
5. How does conjunctival papilloma look?
It typically appears as a fleshy, pink, lobulated, raspberry-like growth on the conjunctiva.
6. Is conjunctival papilloma painful?
Most cases are painless, though some patients may report mild irritation or foreign-body sensation.
7. Should conjunctival papilloma be removed?
Removal is recommended if:
- The lesion is growing
- Suspicious for malignancy
- Causing irritation
- Cosmetically bothersome
